On June 7th, the Soho forum hosted a debate between Jeff Singer and Adriane Fugh-Berman on the opioid epidemic. The resolution was “America's overdose crisis is the result of doctors over‐treating patients with opioids.” Adriane argued for the affirmative, Jeff took the negative. (I refer to Jeff by his first name because I have had several friendly conversations with him, and I refer to Adriane by her first name for symmetry.) You can watch the full event here, or most likely you can find it on your favorite podcast app. I will share my thoughts on the event below.
I won't pretend to be neutral. People who have followed me for a while know I have strong opinions on this. My most comprehensive post on this topic is here, and see here for a Cato paper that I helped with, which was authored by Jeff Miron and Laura Nicolae. I think Jeff won the debate handily. Adriane said a lot of things that are patently untrue and spins an implausible narrative of pharmaceutical companies successfully bamboozling doctors and patients. Her general story doesn't make any sense, and I think there is a very important key fact that blows apart her narrative. Jeff hits her with this crucial information, and she failed to deal with it in any material way.
By Oxford rules the debate was a tie. But there were partisans of both sides in the audience, and they tend to pretend they're undecided at the beginning and "change their minds" later to agree with their champion. At first I thought, "How in the hell is this a tie?!", but I spoke with Jeff by phone and he explained that this often happens in Oxford-style debates.
[Note: I tried to quote or paraphrase accurately. I apologize if something that appears in quotes isn't the exact wording they used in the debate. I made my best effort to quote verbatim, but I did not have a written transcript to work from. If there are any instances of me quote/paraphrasing and changing the meaning of what someone said, I will correct it in the post.]
Effectiveness of Opioids for Chronic Pain Relief
The most insane thing that Adriane claims is that opioids are not effective at all for chronic pain. She concedes that they are sometimes effective for acute pain and for end of life pain. But this makes no sense. If opioids can relieve cancer pain (which is chronic pain, assuming most cancer patients live for a few months or years after diagnosis), they can relieve other kinds of pain that result from, say, degrading joints or musculoskeletal issues. Adriane's story is that chronic pain patients develop a tolerance to opioids, so they stop working unless they keep increasing the dose. They can even develop "hyperalgesia", an extreme sensitivity to pain. All of that is likely true, but no doubt there are still millions of chronic pain sufferers who only get relief from opioids. Some of these patients are forced to taper off opioids because their doctors, concerned about criminal liability, become uncomfortable treating pain patients with high dose prescriptions. And sometimes these patients experience such awful pain as a consequence that they end up committing suicide. Some "pain refugees" flee across state borders to get relief. I'm tempted to believe these people when they tell us that they are getting some kind of relief from opioids.
There is a more reasonable version of the claim Adriane is making (though it's clearly not the reasonable version she espouses). One could argue that opioids do work for chronic pain, but they don't pass the cost-benefit test because of the associated risks. In other words, a terminal cancer patient doesn't have much to lose, but someone with musculoskeletal aches and pains potentially has a long, healthy life ahead of them. There is certainly merit to this kind of argument, but Adriane is claiming that opioids don't work at all for the latter kind of pain patient. Why wouldn't the cancer patient gradually develop tolerance to the opioids until they stop working? Presumably you could have bad cancer-related pain but still survive for months or years. I think she's probably correct with respect to some kinds of chronic pain. Headaches, for example, tend to result in bad rebound pain when opioids are used for relief. But some sources of chronic pain are similar to cancer in the sense that something in the body is badly out of place and triggering the nervous system.
Jeff was reluctant to engage on this point because it was in his opinion a side-show, not necessarily germane to the resolution. But re-read the resolution's exact language, it specifies that "over-prescription" of opioids is the cause of the epidemic. I think this inserts a value judgment or clinical judgment over whether the increase in opioid prescriptions over time was justified. Jeff responded by pointing out that there is an ongoing debate among clinicians over how effective opioids are at treating chronic pain, and it's facile of Adriane to just assert that the case is closed based on some evidence that she happens to like. (In one exchange Jeff says, "Do I have to be dying to get pain relief!" to which Adriane replies, "But it doesn't work!")
This theme of the debate highlights a difference in worldviews, which I think could be it's own separate forum debate. Adriane has a technocratic worldview. If I understand correctly, she is not a practicing physician but is rather an academic researcher (still an MD, and still a valid perspective, it's just a different view of the landscape). Decisive answers can be reached using The Science ™ (my characterization, not hers). She has no respect for practicing clinicians who don't share her conclusions. (This doesn't come through strongly in the debate, but in her paid testimony in the Oklahoma opioid lawsuit she was asked a question about doctors disagreeing on this point. She responded: "Medical professionals may disagree on this, but the science on it is quite clear." Clearly she thinks she has access to ways of knowing that are superior to the mere anecdotes and inferences of her colleagues who practice medicine for a living.) She cites some randomized controlled trials and meta analyses that supposedly prove opioids aren't effective. I have not done an extensive literature review on this, but the first couple of meta studies I find in a Google search for "opioids for chronic pain meta study" seem to indicate that they are effective. (Though they also show there are some negative side effects, and sometimes non-significant improvements over NSAIDs and other pain relievers, but it's a lie to say that they don't work at all.) But let's suppose there are some really good RCTs that show no lasting benefit of opioids on chronic pain relief. Here's why that shouldn't matter.
Doing an RCT is essentially admitting that people have different physiologies, that even if the medicine "works" in some general sense, it will work for some patients but not others. In the case of opioids (codeine specifically), we actually know about genetic markers that make some people "fast" or "slow" metabolizers, the latter getting little relief and the former being incredibly sensitive to even low doses. It's easy to imagine a scenario where you run an RCT that implicitly models everyone as being the same. (It's weird how scientific studies sometimes sneak in assumptions that are bat-shit crazy if you say them out loud.) You give everyone in the treatment group the same regimen of opioids for pain relief. Some, say 1/3, get no relief, because maybe they're slow metabolizers. Another third get relief from chronic pain for the first time in their lives and are happy they've finally found a solution to their soul-crushing pain. The remaining third gets "rebound pain". Maybe they quickly metabolize the opioids and the acute withdrawal makes their pain worse. Maybe the signal from the 1/3 for whom it's effective is cancelled by the 1/3 for whom the pain is worse, or maybe it doesn't exactly cancel but the average effect gets pushed into "non-significant" territory. It's easy to imagine a scenario where you get a null result, or even a result in which you've "proved" that opioids make chronic pain worse. This approach to the truth is something that's pretending to be science, but it actually ignores most of what we know about human variability. The RCT is implicitly pretending everyone is the physiologically the same, that a treatment that objectively "works" may not work for some individuals due only to unobservable random factors, and that simply gathering enough data points to shake out the noise will yield the true signal.
In the real world, chronic pain treatment can be a lifelong journey. The sufferer may try various remedies: physical therapy, orthopedics, over-the-counter pain medicine. If none of these work, it's perfectly appropriate to try opioids. If these chronic pain sufferers, who have already tried all the other options, suddenly and persistently get relief from opioids, my inclination is to believe them. Their physicians, who suddenly see an improvement in their patients ability to function, aren't being fooled by randomness or by an overactive pattern-matching routine running in their brains. They should not feel the need to correct their anecdotal inferences with the "hard data" coming from RCTs. What I have described above is an individualized fine-tuning of a treatment regime. For chronic conditions, including chronic pain, it looks really telling when the patient's persistent condition turns on a dime under a new treatment regimen. RCTs are nice, but in this case there are good reasons to doubt them.* Please note that this isn't a general case against RCTs. I gave specific reasons to doubt them, including known variability in our physiological ability to process opioids (in this case with known genetic variations explaining the difference), the subjectivity of the outcome, and the ability to detect effectiveness of a treatment within an individual.
Adriane does say something about chronic pain management that I agree with. Exercise is often found to be the most powerful treatment, she cites some evidence to this effect. This makes intuitive sense to me. A lot of people have chronic pain issues from being overweight, which puts a strain on joints and the back. A combination of weight loss and (perhaps just as importantly) strength training can improve their situation by increasing the integrity of the structure while lightening the load. Three cheers for lifestyle interventions! I think there are a lot of chronic pain sufferers who would benefit from substantial lifestyle changes, and I don't just mean exercise and weight loss. There could be dietary factors contributing to inflammation (admittedly there's a lot of junk science and fad diets in this space). Maybe meditation or some kind of mindset adjustment would allow some patients to feel less anxious about their pain. At the same time, exercise is just not an option for some people who are completely immobilized by agonizing pain, or whose joints are so compromised that significant exercise is ruled out. Opioids shouldn't be dismissed for such patients.
Addictiveness and Addiction Rates of Opioids
Adriane vastly overstates the addiction rate of prescription opioids. She makes categorical statements such as "No one is immune", "All opioids are addictive", "All opioids cause death." Her preferred estimate of the addiction rate is "8-12%", at one point saying up to 1/3 of prescription opioid users become addicted. All of this is in service of attacking the pharmaceutical companies' marketing campaign, which asserted that rates of addiction were somewhere in the area of 1%. (The pharmaceutical companies are actually in the right ballpark here, and Adriane is way off base.)
Jeff cites some much lower estimates for the rates of addiction among opioid users. He cites multiple Cochran studies that show abuse and addiction rates among opioid patients is quite low. One study found misuse rates at 0.6%. Addiction must be rarer still, given that the occasional misuser of opioids is not necessarily an addict.
Adriane herself cites the infamous Porter and Jick paper, which found only 4 addicted patients out of 11,882 who were given a narcotic (1 case was thought to be severe), though her motive was to mock it as nonsensical. Much ink is spilt over this paper and how it was supposedly misused by pharmaceutical companies and pain doctors to "understate" the addiction risk. I insist that this paper is still telling evidence that addiction is rare. This paper comes up with a low estimate for the rate of addiction compared to other more recent papers. But if opioids had the power to pharmacologically enslave users that Adriane is insisting upon, there's no way in hell they'd get anything that low.
What the hell is going on here? How could there be such a broad range of estimates? Who's right? My short answer is that the low estimates are right and the higher estimates are not remotely plausible. Addiction rates are low, in the ballpark of 1%.
As I describe in a previous post, you can find this broad range of estimates within a single paper that's measuring different things and reporting different estimates. There lies the key. Here is a paper that finds addiction arising in 0.19% of cases of patients with no history of opioid abuse. Aberrant behavior occurs in 11.5% of cases, but this drops to 0.59% when pre-selecting for people with no history of abuse. I think that filtering out pre-existing abuse is what's separating the high estimates from the low estimates. (See below, Adriane is also entertaining an overly broad definition of "addiction" that conflates problematic drug use with physical dependency.) Let's insert an obvious fact here: People who are addicted to opioids prefer a steady, legal supply and try very hard to get this from their doctor. Doctors attempt to screen for this, but no sorting mechanism is 100% effective. So contra Adriane's story, it is simply not the case that opioid-naïve patients are getting addicted to their legal prescriptions in large numbers. More likely, her preferred estimates arise from the phenomenon of existing addicts seeking a supply and occasionally getting a prescription. This is really freaking important if you want to understand these numbers. If you're asking the question, "What fraction of opioid patients are addicts?" then maybe the answer shifts closer to Adriane's estimates. But if the question is, "What is the chance that an opioid-naïve patient will become an addict, given that I start them on an opioid?" the answer is closer to Jeff's estimates. The latter question is the one that's relevant to weighing the risks and trade-offs associated with starting someone on a potentially dangerous medicine, the former is a completely irrelevant exercise in dividing one number by another number.
(Here is another paper that gets a 0.6% figure, which is the number Jeff gives in his opening statement.)
There is another reason to think that the lower figures are more plausible. We have population-level measures of addiction and misuse rates. In my Dreamland post, I do some math based on numbers from the SAMHSA surveys on drug use. There were about 97 million past-year opioid users and 2 million people who'd had an opioid use disorder in the past year. Naively dividing one by the other gets about 2%. But (and Jeff cites this figure in his opening statement) only about 1/4 to 1/5 of opioid abusers have or ever had a legitimate medical prescription. Most are getting their supply from a dealer, friend, or family member. So it's really only about 0.5 million or so of those addicts who started off as prescription opioid users. So, taking a very crude estimate, 0.5 million over 97 million is about 0.5%, which is suspiciously close to the number found in a couple of the papers linked to above and the paper cited by Jeff. The population-level back-of-the-envelope in this paragraph is admittedly crude. There is no accounting for the journey over time to becoming an addict, as I am just using a snapshot in time based on a single year's data. But the population level numbers absolutely rule out the larger estimates that Adriane gives, unless the SAMHSA figures are off by orders of magnitude. (I'm happy to say that a survey will miss a lot of people, say homeless people or folks without a consistent address. But is it off by a factor of ten? And anyway I have seen peddlers of the standard opioid narrative cite these figures uncritically, so presumably they don't take issues with their accuracy. If there are better estimates that attempt to correct for the shortcomings of the SAMHSA survey results, I'm happy to entertain them.)
Multi-Drug Poisonings
Jeff really hammers on the issue of multi-drug poisonings. I have written about this many times. The point here is that most "opioid overdoses" are not single-drug poisonings. The toxicology often returns multiple substances, many of which are known to have interactions with opioids. Benzodiazepines, for example, are pretty harmless by themselves (from an overdose perspective anyway), but can potentiate the effect of opioids. Jeff says: Doctors aren't prescribing cocktails of opioids, benzodiazepines, and cocaine. He points out that the "opioids pharmacologically dominate the will" story doesn't make any sense in this context. It would make sense if opioid addiction were driving people to gobble down higher and higher doses of opioids until they finally overdose. But there is no reason to think a physical dependence on opioids is going to cause you to seek out other kinds of drugs. This piece of evidence militates against the purely pharmacological account of addiction and in favor of a behavioral theory a la Unbroken Brain by Maia Szalavitz. In light of this evidence, the story of adults with bad habits and poor coping mechanisms seeking out available methods of getting high is more plausible than the story of normal, well-adjusted people getting enslaved by a chemical.
Adriane answers (around the 37 minute mark), but not in a satisfying way. She seems to admit that benzos can potentiate opioids and it's the combination that kills you. But she also seems to say that it's the opioids that kill you, not the other drugs in the toxicology screening. ("If somebody pinches you and then shoots you, it's the bullet that kills you.") Maybe she was admitting the point about benzos but making a different assertion when it's other combinations? It was a very confused response, and she didn't seem to respond to the point that opioid addiction should not cause someone to use other recreational drugs. Jeff's point stands: Opioids are far less dangerous and have far less power to enslave the will than what Adriane is implying.
Addiction versus Physical Dependence
Jeff does his best to draw the distinction between addiction and physical dependence. Physical dependence is a physiological response to a chemical, which entails tolerance and withdrawal symptoms. Addiction is a behavioral term, which means continued use despite negative consequences. He uses the neutral example of beta blockers, which can effectively control high blood pressure in some patients. However, going off beta blockers suddenly can cause dangerously high blood pressure and potentially deadly heart rhythms. No one would characterize such a patient as an "addict", even if this patient has been treated with beta blockers for years and is completely dependent on them. And no one would impart a moral dimension to their dependence or to a sudden fatal withdrawal.
I think Maia Szalavitz's addiction experience is relevant here, because she presents a case of addiction persisting in the absence of physical dependence. (Not mentioned during the debate.) She was arrested and forced into treatment, even being forced into a state of withdrawal by a dose of naloxone (a treatment for which she had not given informed consent). She was eventually released from jail. She came out of the experience "clean" in a physiological sense, in that the withdrawal symptoms had stopped. Her body was no longer dependent on the substance, and presumably her tolerance had returned to baseline. But she still had a psychological need for the drug. She was desperate to get back to her stash of dilaudid (an opioid) that she knew the cops hadn't found. It was a habit she'd developed, but it was not due to "chemical hooks" in the substance itself. In contrast, some people might experience withdrawal symptoms after completing a course of opioids and never even associate the symptoms with the substance. The compulsion to seek more and the physical withdrawal are distinct entities.
Adriane does her best to elide the difference. She never really concedes that these are different animals. It's not just a careless omission, either. She at times explicitly blurs the distinction. In her opening remarks around the 11 minute mark, she says that the terms "tolerance" and "dependence" were "coopted" by the pharmaceutical companies. I think this is absolute nonsense. There really was a period where doctors were afraid of opioids and they really didn't distinguish properly between problematic addiction and physiological dependence. If anyone led a campaign to correct this blind spot in their thinking, they provided an important public service. (It wasn't just pharmaceutical companies, either! There were some very concerned physicians who were worried about the undertreatment of chronic pain.) I read this as Adriane trying to dismiss an important concept that's inconvenient to her argument. There really isn't a charitable reading, in my opinion.
I think this also might explain Adriane's higher estimate for the risk of "addiction." If you're using a definition that's so broad it encompasses things that aren't really addiction, you'll naturally get a higher figure. Probably everybody who does a course of long-term opioids experiences some kind of withdrawal when they go off. And sometimes it's quite unpleasant, I don't want to dismiss their pain. (I, for one, am not in the business of dismissing other people's serious discomfort.) But it's not the same thing as addiction, and conflating them is inexcusable.
Disconnect Between Prescribing Rates and Addiction and Drug Overdose Rates
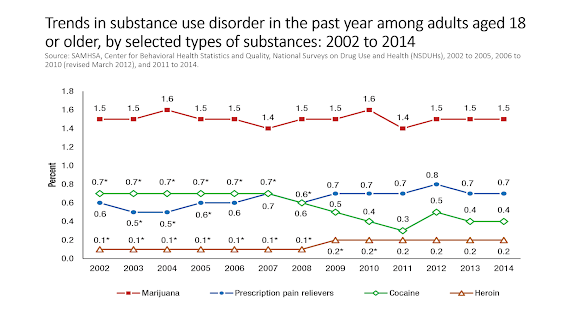
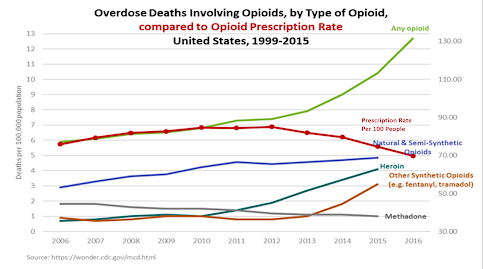
Jeff had some very good slides which make a point I have blogged about before. You can see them if you watch the video posted at the top, but I'll reproduce a couple of them here. The first shows a time series of addiction rates from 2002 to 2014. If you fit a regression line to the blue curve, which shows the addiction rate for prescription painkillers, you may get a mildly positive trend. But it starts at 0.6% and ends at 0.7%. In other words, it's basically flat. This kills the narrative. Adriane's story is that loose prescribing led to a growing population of addicts, and with more addicts there are naturally more overdoses. (And I'm not picking on her, this is the standard narrative peddled by opioid alarmists.) She does concede that the recent skyrocketing death rates are due to people switching from prescription pills to heroin and fentanyl, but she doesn't seem to realize this is a concession to Jeff's worldview. That is, but for prohibition, the addicts could have maintained themselves on a relatively steady, high-quality supply rather than switching to a black market with wildly, unpredictably fluctuating potency.
How Gullible Are Doctors?
Adriane's worldview is incredibly cynical, bordering on paranoid. In her view, pharmaceutical companies have incredibly insidious influence over the way medicine is practiced. Their advertisements and their attempts to influence doctors are extremely powerful, and doctors don't realize they're being bamboozled. She refers to "fairytales" told by the pharmaceutical companies, specifically in reference to the lower estimates of addiction (which it turns out are correct). She even smears one of the questioners during the Q&A, Josh Bloom of the American Council on Science and Health. (She insinuates that his organization is tainted by pharmaceutical money, to which he responds "That's a lie." Epstein quickly moves on to the next question, but it's a pretty ugly encounter.)
I think this stuff is catnip for left-wing and right-wing audiences. For the left, this is an opportunity to reflexively raise a middle finger to corporate America. Their greed is so immense they don't care how many bodies they leave in their wake in pursuit of profit. For right-wingers with a puritanical bent, we have a massive drug peddler finally getting its comeuppance. Unfortunately it's all nonsense. I see Adriane as playing to her audience's knee-jerk political instincts (something we all need to stop falling for).
Part of this story is that pharmaceutical companies are well-resourced and adept at manipulating people. Unfortunately for this narrative, it's actually really difficult to fool people consistently. If you think someone is getting one over on you, or if you sense that they have any incentive to mislead, you will instinctively discount anything they say. Even unsophisticated people who sense that someone is trying to fast-talk them can simply tune out their would-be manipulator. This places an upper limit on how convincing any argument or ad campaign can actually be, no matter how slick or well-funded. The notion of these corporate behemoths running roughshod over mindless sheep is a fantasy. Keep in mind that these are doctors! Sure, some doctors are gullible. Some may occasionally say embarrassingly foolish things in public. But most are pretty smart. They are basically the most scientifically educated class of people in society. And the people who are trying to mislead them are often drug reps with no scientific background. I say the doctors have the advantage in this encounter. (Sometimes the influencers are doctors who are paid by the pharmaceutical company to deliver lectures or "continuing education." But most drug reps are not, many have little scientific training and are basically charismatic people following a script. I know about studies showing that doctors commonly make elementary math and statistics errors, some of which are relevant to the practice of medicine. I readily concede that this is a problem. But they're mostly well equipped to resist the utter sophistry of a slick ad campaign with no actual substance behind it.)
Jeff takes exception to Adriane's characterization of doctors as gullible. He says how implausible it is that a doctor will change their prescribing habits based on a free meal or a pen with a drug's logo on it. They're not so easily bought off or fooled, he insists. In response, Adriane again shows her technocratic side. She goes on a long, irrelevant lecture about how small gifts work better than big gifts. Smaller gifts convince the recipient that they did whatever they did for internal reasons, because nobody wants to feel like they were bought off by a trinket or a trivial sum of money. I think this is a cute description of a lab experiment, but once again it's not the real world. The subjects in the experiment she's describing presumably cooperated with the experimental design. In the real world, you can walk away from such noise. You can tune out someone who's trying to snow you, and this is exactly what we do.
This doesn't get mentioned during the debate, but here is my write-up of a study about the supposed origins of the opioid epidemic. It attempts to blame state-by-state differences in overdose rates with Purdue Pharma's marketing campaign, which varied by state based on the paperwork burden of prescribing opioids. There are a lot of serious problems with the paper. It's interesting that this is the academic attempt to rigorously make the argument that anti-opioid crusaders are making more anecdotally, and it ultimately falls flat. Also notable, it's funny how Purdue is blamed for creating a market that is more than 10x it's own market share. They're a bit player in their own industry, following a trend but not creating it out of thin air.
Other Notable Moments
I'll end with some unconnected thoughts about a few interesting moments during the debate.
Stanton Peele asks the first question in the Q&A, and he kind of makes an ass of himself. It's unfortunate, because I actually really like Stanton. He tries to poll the audience as to how many of them have ever taken an opioid, by a show of hands, and tries to follow it up with how many of them had a problem going off them. Jacob Sullum did the same thing in his debate with Alex Berenson a few years ago (my write-up of that debate is here, but it's worth watching the full debate too). You can't see the audience, but a very large number of people raised their hands to the "were you ever prescribed a course of opioids" question and almost nobody raised their hands to "Did you have some problems coming off them?". (Was it exactly zero people? We didn't get an official tally.) I think the debaters can do this, but it's probably obnoxious for a questioner to do the same. Epstein, the moderator, cut him off as Peele shouts something (to someone, it's not clear who he's yelling at). I think the voters in these debates aren't necessarily just voting on who best defended their position according to the precise wording of the resolution. Sometimes they are swayed by things like demeanor, charisma, unrelated topics that are tangential to the resolution, etc.. Stanton's behavior is likely to turn away marginal voters, who look at this and say, "These guys are a bunch of crazies." We need to keep our crazy zealots in check.
During the Q&A Jeff responds to a question about a policy of over-the-counter availability for essentially any drug. I think it was meant as some kind of "gotcha", but Jeff handles it well. I don't know how this comes off to an uninitiated audience. It may be bad strategy from the standpoint of winning an Oxford-style debate. As in, the borderline voters may think you're a crazy bastard for taking an extreme position, so they may discount the rest of your arguments (even based on something that's not necessarily germane to the resolution). On the other hand, there's a "long game" to play here. This debate may have been some audience members' first exposure to libertarian ideas, or to the concept of bodily autonomy and self-ownership as moral principles. (Principles that are not universally recognized, unfortunately.) One could even lose the debate while winning the long game, because these ideas will stick in some people's minds and germinate. On this specific point, I actually think it's a moral imperative that we allow opioids to be available over the counter to anyone who asks for them. Currently we have a system of gatekeepers, doctors and pharmacists, who stand between pain sufferers and pain relief. This means that doctors can suddenly stop prescribing opioids to a pain patient who has been using them for years. Maybe the doctor is afraid of legal scrutiny, as in law enforcement deciding that they are prescribing too much. Or maybe the doctor literally gets arrested and charged, and his pain patients are left out in the cold without a provider. Something like this is happening today. It is definitely keeping chronic pain patients from getting the only treatment that works for them.
That brings me to another point. There is some discussion of suicide among opioid patients. Adriane absurdly attributes higher rates of suicide among opioid patients to opioids themselves. It's another absurd dismissal of human agency in favor of voodoo pharmacology, as if the chemicals themselves are driving behavior. Jeff calls her out on it, saying that the causal connection isn't the one Adriane is implying. Jeff gives the more plausible reading of these numbers: chronic pain patients tend to be suicidal because chronic pain can be a living hell. It's kind of funny, because Adriane dumps on some of the studies Jeff cites as being "observational" and not sufficiently rigorous in terms of proving causation. But this is a case of her making the "correlation is causation" fallacy, even when there's a much more plausible story.
That's the end of my commentary on the debate itself, but I really need to share this video of Adriane giving a speaker a hard time at what appears to be some kind of medical conference. I think it speaks really poorly of her character and lays bare her underlying motives. The speaker, Stephen Kertesz, presents reams of evidence of patients who have committed suicide because of a "forced taper", meaning their physicians involuntarily cutting their opioid dose. Because the government doesn't collect data on this, one has to turn to collecting anecdotes and news reports. Adriane is obviously not happy with the talk. (Do watch the whole thing, tell me if I'm being unfair.) Kertesz isn't trying to deliver a slam-dunk conclusion. He's ultimately arguing for the collection of data that would allow the government to track how much and how often this is happening. Adriane pushes back against even that modest proposal of collecting the data. She absurdly insists that there isn't evidence of a huge surge in such suicides, and the speaker quite fairly points out that this is a kind of Catch-22. As in: Yeah, there's no evidence of a huge surge because we're not collecting the data! Kertesz actually does an excellent job of collecting whatever sparse data is available, scraping news stories, interviewing spouses, social media posts and such. What kind of evidence does Adriane expect to see if official numbers aren't being tabulated? What would be the difference between a "large signal" and a "small signal", in her view, without such tabulation? Once again, it's really hard for me to interpret her behavior charitably. Adriane is a board member of PROP, the "Physicians for Responsible Opioid Prescribing". This group very likely helped write the CDC's disastrous opioid prescribing guidelines. These guidelines, while nominally just providing "guidance", in reality had the force of law behind them and were used to red-flag physicians who were overprescribing. Maximum "recommended" doses listed in the guidelines were interpreted by physicians, who were astute about reading the temperature in the room, as hard cut-offs. It led to a lot of forced tapers. Adriane is in denial about this, "Who is calling for a forced taper?" she says. It's pretty clear she's being defensive and deflecting blame. Obviously she'd be hostile to any attempt to uncover the bodies. An honest player here would say, "Go ahead, collect the data. You'll see this is a big nothingburger, but it's worth the modest expense at data collection." Instead she's adopted this strategy of castigating her colleagues at professional conferences for bringing up the topic. Kertesz responds admirably to this abuse. My takeaway here is that Adriane is not an honest broker of the truth. She's just as compromised by a combination of financial incentives (she is a paid witness) and her partisanship in an anti-opioid crusade. Money isn't the only thing that can compromise a person's integrity. If there is any chance at all that opioid policy is torturing people to the point of suicide, then we should be incurring whatever expense is necessary to collect the data. (Does Adriane see herself as the guardian of scarce research dollars, simply guarding against profligate spending on someone's hunch? I really have a hard time reading a pure motive in this exchange.) There are some actual studies of this question using large sample sizes, by the way, so Kertesz isn't merely falling for a few emotional anecdotes.
There was some discussion during the Q&A about why pain patients aren't more organized. I would like to hear more directly from them at events like this. I see Adriane as completely dismissing these people. She asserts that opioids don't work for chronic pain. I'd like to see the chronic pain patient who has successfully regained their functionality to approach the mic at one of these events and say, "I understand you don't believe I exist..." It doesn't have to be mean. Nobody has to shout her down, use harsh language, or make a scene. Such tactics can even be counterproductive. There's no need to even raise one's voice. I think a steady drumbeat of chronic pain suffers, each calmly recounting how their life was a living hell without opioids, would make the point just fine. My understanding is that there is adequate security at the Soho forum to avoid rowdy disruptions, so that might be why we didn't see these chronic pain sufferers screaming in Adriane's face. And I really don't want to see that. Adriane is in some sense simply serving as the avatar for a commonly believed narrative. It's important to create forums where such people can share their perspective without fear of being shouted down or drenched with spittle-laden invective. At the same time, if her perspective wins it means some chronic pain patients will be tortured to the point of suicide. I think she needs to be brought face-to-face with this.
___________________________________________
*I want to run an RCT where I randomly switch out items from someone's shopping cart at a grocery store. The customer protests, "But, I love Wishbone Creamy Caesar dressing!" Scientist replies, "Sorry, but RCTs have found no improvement in general happiness comparing Caesar dressing users to over-the-counter Ranch users. Congratulations, you're in the control group of a follow up RCT! Ranch for you!" Sometimes medicine is like chemistry. It just works, and it works the same for all of us because we have roughly the same physiology. But sometimes it's more like a shopping basket, where you've built up preferences and patterns over the course of a lifetime and you've figured out what works for you. For something as subjective as pain, I think it's more like a shopping basket than a test tube.

No comments:
Post a Comment